- Your cart is empty
- Continuer mes achats
Product Description
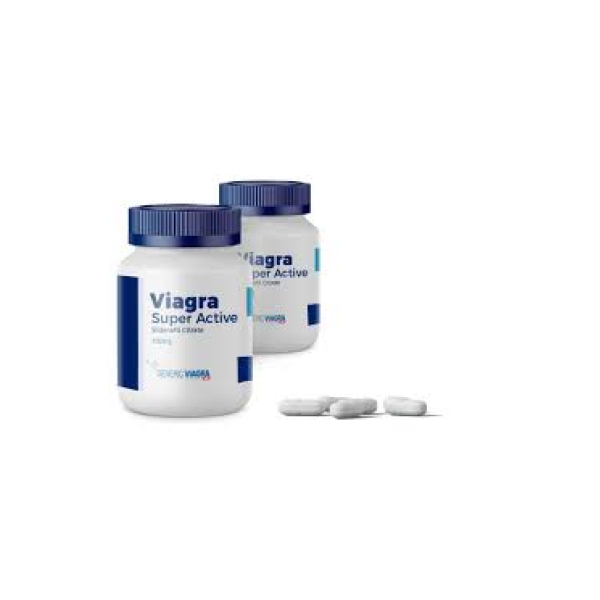
La perception du Viagra par le public est positive. Il n’est donc pas surprenant que le Viagra Super Active soit présenté par les fabricants comme une substance améliorée du médicament original. Vous avez certainement entendu parler du Viagra comme d’un médicament de “nouvelle génération”. Toutefois, si vous n’en avez pas entendu parler, vous êtes peut-être curieux de savoir ce qu’est le Viagra Super Active.
Le Viagra en est à sa quatrième version et cette fois, il s’appelle Viagra Super Active. La formule pour créer le Viagra Super Active est légèrement différente de celle du médicament original, mais il est toujours considéré comme un inhibiteur des phosphodiestérases connu pour traiter la dysfonction érectile. Ce médicament est généralement pris sous forme orale. En général, le Viagra Super Active est pris avant l’activité sexuelle comme méthode pour obtenir et maintenir une érection. Le Viagra en général est considéré comme un médicament sûr, et toutes les versions précédentes sont également fiables, sûres et utiles pour traiter la dysfonction érectile.
Quel est le meilleur moment pour prendre Viagra Super Active ?
Contrairement aux autres versions connues de Viagra, Viagra Super Active est distribué sous la forme d’une pilule de gélatine. Les autres comprimés se présentent sous une formule dure. La pilule de gélatine est molle et se dissout immédiatement une fois qu’elle est dans votre système. Viagra Super Active est absorbé rapidement dans votre sang, ce qui fait que les ingrédients agissent plus vite et produisent des résultats plus rapides. Cela signifie qu’il y aura un meilleur délai d’exécution, pour ainsi dire, entre la consommation de la pilule et le rapport sexuel.
Viagra Super Active doit être pris uniquement lorsque cela est nécessaire. Par exemple, vous pouvez le prendre entre 30 et 60 minutes avant le rapport sexuel. Le sildénafil circule dans votre sang pendant quatre heures au maximum, puis il est complètement éliminé de votre système. Cette pilule ne doit être prise qu’une fois par jour.
Comment fonctionne le Viagra Super Active et quelle est son efficacité ?
Il y a un avantage à prendre Viagra Super Active plutôt que les médicaments d’autres générations. On dit que cette formule est plus fiable et plus sûre que les formules précédentes. On dit que le Viagra Super Active a des effets plus importants à l’intérieur du corps, ce qui fait que les vaisseaux sanguins font plus de place au pénis, déclenchant une érection en permettant au sang d’entrer directement.
Il y a tellement de raisons pour lesquelles de plus en plus de personnes choisissent de prendre Viagra Super Active. Outre sa capacité à résoudre les problèmes de dysfonctionnement érectile, il existe d’autres facteurs qui font de Viagra Super Active le médicament le plus préféré. Selon les recherches, Viagra Super Active a été spécialement formulé pour fonctionner en toute sécurité – même avec d’autres médicaments. C’est une bonne nouvelle pour ceux qui ont des problèmes de santé tels que l’insuffisance cardiaque congestive. Alors que les autres médicaments contre la dysfonction érectile ne sont pas idéaux pour être pris avec des médicaments pour le cœur, Viagra Super Active est une exception.
Effets secondaires
Il est possible de ressentir des effets secondaires légers à modérés après la consommation de la variante Super Active du Viagra, tels que :
- Maux de tête
- Bouffées de chaleur (rougeur, chaleur)
- Indigestion
- Troubles respiratoires et des voies urinaires
- Troubles visuels, flou et perte de la vision
- Perte de l’ouïe
- Étourdissements et vertiges
- Sonnerie ou bourdonnement dans les oreilles
- Congestion nasale
- Palpitations
- Érection douloureuse et prolongée
Remarque : Si une érection se prolonge pendant plus de 4 heures, vous devez consulter immédiatement votre médecin.
Comment cela fonctionne-t-il ?
L’effet de tout type de Viagra repose sur le sildénafil : il bloque les inhibiteurs de la PDE5 afin de maintenir le flux sanguin vers les muscles du pénis et de les garder détendus. Mais lorsqu’il s’agit du Viagra Super Active, l’effet est tout simplement plus fort. Tout d’abord, il stimule le flux sanguin vers les tissus péniens et permet de maintenir une érection pendant 8 heures au lieu de 4 !
Deuxièmement, le médicament est généralement excellent pour la santé masculine – il aide à rétablir des fonctions sexuelles normales et à reprendre le dessus. Certains experts disent aussi que le Viagra normalise le niveau de testostérone dans le sang – c’est utile pour la vie sexuelle et le bien-être général, aussi. En d’autres termes, Viagra Super Active est un médicament plus puissant qui aide l’homme à être un homme.
Devrais-je l’essayer ?
Ce produit a été créé pour les hommes adultes confrontés à des problèmes d’érection et de courte durée des rapports sexuels. Etant un médicament générique, Viagra Super Active n’est pas officiellement prescrit par les médecins, mais ce remède est fortement recommandé pour le traitement instantané des problèmes d’érection. Veuillez noter que Viagra Super Active ne doit pas être utilisé par les hommes de moins de 18 ans, et doit être pris très prudemment par les hommes de plus de 65 ans car il a un effet assez fort. Le médicament n’est pas censé être utilisé par les femmes !
- Centre de la perte auditive à Lausanne - 29. juillet 2023
- Inspire-toi - 23. juin 2023
- Epinext – One Mission: Zero Seizures. - 25. avril 2023














Avis
Il n’y a pas encore d’avis.